Pandemic Report: Has Ageism Become the New Eugenics?
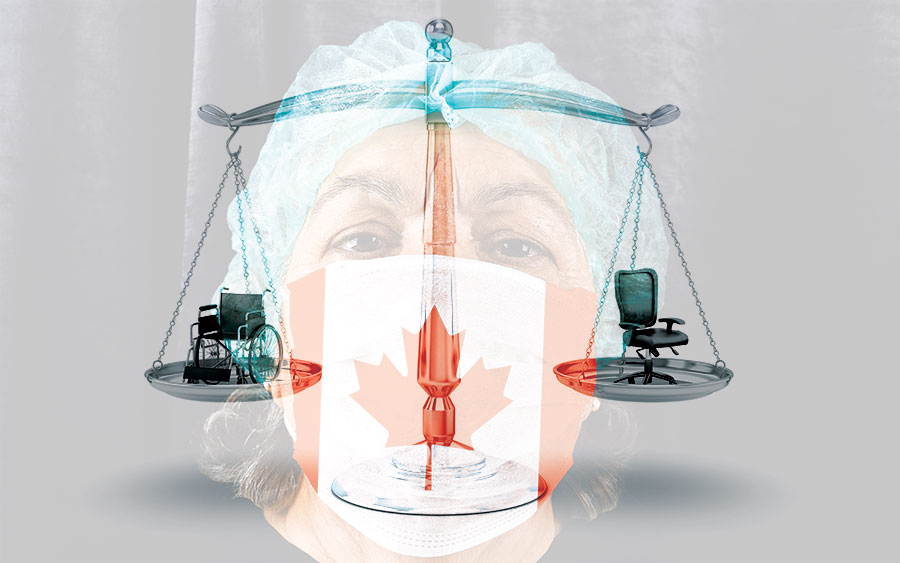
From seniors being denied ventilators to #boomerremover trending online, the COVID-19 global pandemic has exposed the real danger of ageism. Photography: Porcorex/Getty Images (scale); Mustafa Güner/Gettyimages (woman)
Older people have been denied ventilators. Even some suggest they should sacrifice their lives to save the economy and younger people.
It’s hard to imagine how a 70-year-old could become the face of ageism in the 2020 pandemic. But on March 23, Dan Patrick, the lieutenant governor of Texas, told Fox News that grandparents like himself – who are at high risk of dying from COVID-19 – would sacrifice their survival if it would allow America to lift public health restrictions and get back to work. Patrick predicted that he and other seniors would be “smart” about protecting themselves from the novel coronavirus but would willingly gamble their lives to save the economy for their grandchildren.
“If I get sick, I’ll go and try to get better,” he said, “but if I don’t, I don’t.”
About 3,000 kilometres north of Texas, the Republican’s comments lit up the Twitter feed of Erika Dyck, a professor who teaches the history of health and social justice at the University of Saskatchewan in Saskatoon.
Patrick’s view that an older life is worth less than a younger one – and even less than the economy – prompted overwhelming consensus among her fellow historians. “They said, ‘This is eugenics, this is eugenics!’” Dyck, who holds the Canada Research Chair in the History of Medicine, could see their point.
The eugenics movement sprouted out of the 19th-century idea that a desirable society could be genetically sculpted through selective breeding. In the 20th century, it penned some of history’s ugliest chapters: involuntary euthanasia in the U.S., Hitler’s pursuit of racial purity in Nazi Germany and the Holocaust and, in Canada, forced sterilizations and the genocide of Indigenous peoples – all trampling the lives and rights of minorities under the guise of society’s betterment. Amid this 21st-century pandemic, Dyck says the same “for the greater good” arguments are being used to justify the broad devaluation of the elderly.
“With [early] eugenics, decisions were made based on assumptions around people’s value to society. People with intellectual disabilities, for instance, were considered less productive, less likely to contribute,” says Dyck. The ageism that has emerged with the novel coronavirus wields the same “moral judgments and assumptions about people’s capacity to be productive, either in tax-paying ways or other ways we think are important at the moment.”
Linking ageism with eugenics might sound like a stretch, but just two weeks before Patrick’s incendiary remarks, the U.K.’s Daily Telegraph ran an opinion piece, arguing that “COVID-19 might even prove mildly beneficial in the long term by disproportionately culling elderly dependents.” Then, a few weeks later, the U.S. Office of Civil Rights stepped in to squash a disaster-response triage policy in Alabama, which, according to an official complaint, would have withheld potentially life-saving ventilators from the elderly and those with cognitive disabilities.
The well-being of seniors is now so perilous that Human Rights Watch, the New York-based non-governmental organization that investigates human rights abuses around the world, has identified “older people” as a group in jeopardy. In its April report, it urged governments to “respect the rights of older people in their response to the COVID-19 epidemic,” saying they not only face the greater risk of severe illness and death from the disease but also the threat of “discriminatory attitudes and actions.”
From her Toronto-area apartment, where she has lived alone for 22 years, 86-year-old Marie D’Rozario has watched the rise of ageism with horror and sadness. “I feel like I went to sleep and woke up in a nightmare,” D’Rozario says. “The outbreak has cast older people as dispensable.”
The opinion in The Telegraph, one of her favourite papers, touting the virus as a way to cull the elderly, came as a particular blow. “It’s horrible, totally horrible,” she says, “I’m not going to do their crossword puzzle again.”
What haunts D’Rozario is the cold assumption that older people have nothing to contribute, a supposition her life totally upends. After raising four children, she worked as a secretary and, for a decade after retirement, as a teacher’s aid at the local elementary school. Then, in her 80th year, she spent eight months in Uganda where she ghost-wrote the memoirs of an African industrialist – publishing her first book at the age of 82.
“It’s really terrible when people think that just because you are a certain age, you shouldn’t do things anymore,” she says and, even worse, that reaching a certain age makes you less deserving of compassion. And compassion, she feels, was in short supply for many elderly people who died alone of COVID-19 in Canada’s long-term care homes.
“When we were younger, we regarded our elders with such reverence, we cared so much for them. You didn’t feel they were dispensable,” she says. “There’s a heartlessness that’s now been exposed toward older people … and it’s so overt, it’s so widespread.”
From the first days of the outbreak in Wuhan, China, ageism spread like its own contagion. Headlines that were intended to comfort noted “just the elderly” faced the risk of severe illness and death, emboldening spring breakers to pack Florida beaches and families to fly away for March break. As the pathogen slunk around the globe, the morbid hashtag #boomerremover became a popular meme. Yet even after the World Health Organization dubbed the virus a public health emergency, society did not treat it as a serious, actionable threat until it struck younger people and celebrities like NBA star Rudy Gobert, actor Tom Hanks and the prime minister’s wife, Sophie Grégoire Trudeau.
Now, as COVID-19 has proven it can kill humans of any age and overwhelm hospital resources everywhere, older people tend to rank low in triage plans that determine who should be saved first.
In Spain, where critically ill patients died in the waiting rooms of overcrowded hospitals, one doctor reported that staff at her hospital decided a sick 52-year-old woman would not get a ventilator. At the peak of northern Italy’s outbreak, those aged 80 and up were denied ventilators at one hospital, where the cut-off later dropped to 75 as patient numbers ballooned. In a March 18 account published in the New England Journal of Medicine, one of the doctors involved “admitted how ashamed he was to talk about it.”
The Journal itself recently published a guide to rationing health care during COVID-19, and age factors into it. While the paper recommends ventilators should go first to those most likely to survive – regardless of age – it notes the decision should be based not just on saving a life but saving “the most life years,” meaning younger people with a longer life expectancy would have an advantage.
To Dyck, the criteria for rationing critical care during the pandemic is similar to the way Canadian eugenics programs once judged if someone with an intellectual disability should be forced to be sterilized so they couldn’t have children. “I see it as a bit of corollary, about how we made decisions around who makes a good parent [back then] and who is a good contributing member of society and who gets that ventilator [today].”
Dyck sees no malicious intent behind the agonizing triage decisions that loom, only that eugenic-like arguments are at work in deciding who is most valuable to society.
Even before the pandemic broke out, ageism plagued Canada’s health system. A 2019 news report from the Canadian Medical Association Journal found a dire shortage of doctors who specialize in caring for the elderly, and those who do are paid two to three times less than other specialists although they train for the same length of time. Meanwhile, the number of Canadians over 85 is expected to quadruple in the next two decades. Yet the system has so few geriatricians – only about 300 nationwide, and some provinces have only one – that training in the field is unavailable as a standard rotation in medical school, unlike, say, pediatrics. The report says geriatrics tends to be dismissed as depressing work, but it also blames our youth-obsessed culture, noting that a 1978 satirical novel called The House of God, which refers to older people as GOMERs – Get Out of My Emergency Room – is still popular with medical students.
None of this surprises Ramona Kaptyn. “We are so focused on anti-aging and youth, so focused on it that we don’t value elderly people in our society, the experience and wisdom our elders have and what they can teach us.” Kaptyn, the 74-year-old president of the local chapter of CARP, the advocacy group promoting a New Vision of Aging for Canada [a not-for-profit affiliate of ZoomerMedia], in White Rock-Surrey, B.C., sees a health system in which older people can face unacceptable wait times and harsh attitudes.
“Most health professionals are wonderful people. They’re doing their best. But there is ageism, there is discrimination,” she says, “It’s kind of like, ‘Okay, you’re old. Your joints are wearing out. This is happening to a lot of people, you know. Suck it up [and] here are some meds.’”
Kaptyn, a former journalist and educator, waited more than a year in excruciating pain for hip replacement surgery. Her initial specialist felt she didn’t even need the operation, that she should just keep taking the controversial opiate, oxycodone. “I said, ‘I’m in so much pain and I’m on this medication. When will I get it? Will I have to go to emergency and fall down?’ And he literally said, ‘Yes.’”
Only after a second specialist confirmed her hip urgently needed replacing did Kaptyn get the surgery in 2013. And studies show her experience is hardly unique – wait times for hip and knee replacements and cataract surgeries are rising along with demand.
In cancer care, age underlies a troubling disparity in treatment. In 2014, the Canadian Partnership Against Cancer reported that older Canadians with colon, lung and breast cancer do not receive
recommended treatment at the same rate as younger people. While older patients are more likely to have other conditions that make cancer therapies too risky to undergo, the report concluded that this could still not fully explain the age-related treatment gap.
Historically, age was never a factor in triage. Coined in the late 18th century by the surgeon-in-chief to Napoleon’s Imperial Guard, triage was a way to prioritize immediate, urgent and non-urgent care needs among the mass casualties on a battlefield. Over time, it has evolved into the modern health-care system’s method to save the most lives and deliver the best care with finite resources – not on a first-come, first-serve basis but using objective measures to determine who goes to the front of the line in the emergency room or gets a bed in the intensive care unit.
Seniors infected with COVID-19 make up the highest proportion of those in medical need and, by early May, people over age 60 also accounted for more than 90 per cent of the deaths in Canada. With the probability of having other underlying conditions, they’re particularly vulnerable to the virus, says Dr. Roger Wong, a clinical professor of geriatric medicine at the University of British Columbia. But their prognosis is also hampered by a weakened immune system and one that overreacts. “It’s the inability of the immune system to say, ‘Okay, this is enough,’ and it goes on full blast, affecting multiple organs,” says Wong. “So it’s not just the infection. It’s the body’s reaction that’s compounding the problem.”
Even still, a person’s age doesn’t necessarily reveal how well or poorly they will fare. “Age is basically a number. It’s only a number,” Wong says. “If you use it as a cut-off, it doesn’t reflect when someone is aging quite healthily versus someone of a younger age with multiple health conditions.”
A clinical frailty scale is a better way to predict the outcome for an older patient, he says. The homegrown model, developed by geriatrician Kenneth Rockwood at Dalhousie University in Halifax and used widely throughout the world, is considered an objective way to “measure how vulnerable an older person might be, and frailty is determined by many things – physical condition, mental condition and medical history,” says Wong.
It works like a formula that takes into account a person’s health assets, such as their abilities, and deficits, such as underlying conditions, and returns
a score between one and nine: one is described as “very fit,” while eight is “very severely frail” and nine is “terminally ill.”
“The more frail a person is, the lower the chance of survival in hospital will be,” says Wong, who stresses that decisions around rationing care in these
unprecedented times have to be based on methods, like this one, that are “scientifically sound, practical and compassionate.”
In Ontario, the clinical frailty scale is to be part of the assessment in deciding how to allocate scarce medical resources. Michael Szego, director of the Centre for Clinical Ethics at Unity Health, which represents St. Joseph’s Health Centre, St. Michael’s Hospital and a rehab facility called Providence Healthcare, says the province recently issued a three-stage triage policy for hospital ICUs to follow if patient numbers exceed resources and medical equipment.
In the first stage of rationing, says Szego, those predicted to have an 80 per cent chance of dying based on 13 clinical indicators – including age, blood pressure, respiratory rate and the clinical frailty scale score – would not get a ventilator. In the second stage, those with a 50 per cent chance of dying would be denied. But in the third stage of triage – the worst-case scenario where critically ill patients utterly overwhelm hospital capacity – even those with just a 30 per cent chance of dying would not receive a ventilator.
“I really hope we never get to that [third] stage. That would mean even if you had a 70 per cent chance of surviving, you wouldn’t get a ventilator,” says Szego. “Really, we don’t want to get to any of these stages, but we’re planning for a situation where we have to make those hard decisions. This is very much a reality.”
Before the pandemic, managing scarce resources was largely a matter of logistics. In Canada, most intensive care units operate at 80 to 90 per cent capacity and, for at least 60 days a year, they’re over capacity, says Dr. Timothy Christie, the regional director of ethics services at Horizon Health Network, a hospital corporation in New Brunswick that includes 103 facilities. “We might postpone or delay elective or scheduled surgeries. We might transfer people out of ICU or try to discharge people early from the hospital,” he says, “But this is not like that.
“This is an unprecedented situation. It’s what philosophers have been talking about for years, what we’ve been talking about in the classroom, hypothetically, abstractly debating … now these extreme examples of theory might actually be coming into reality.”
To prepare medical staff for the tough choices that may lie ahead, Christie and his team will rely on a two-tier framework to guide unbiased decision-making. He has seen, for example, “some people advocating for, say, an age cut-off when it comes to getting a ventilator,” but the framework does not directly take age into account.
Instead, it holds that the first issue to determine is which patients have the best chance of survival, regardless of age, because the goal is to save the most lives. “Let’s say you have a 70-year-old patient who has been running and exercising every day of his life, but now he’s sick with corona and he needs a ventilator. Then you also have a patient who is 35, 150 pounds overweight with Type 2 diabetes, a chain smoker who has never exercised a day in his or her life,” Christie says. “In that case, if you look at age only, you’re going to miss the whole picture … that’s where I would say that age is not really the most relevant consideration.”
But if you have two patients who both have the same chance of survival, “The decision should be arbitrary,” he says, as impartial as flipping a coin. The framework also builds in “transparency and accountability,” with plans to document all decisions and in a post-mortem explore how and why they were made.
As with any ethical dilemma, there may not be one right answer and no such thing as a truly arbitrary one. As Christie acknowledges, “None of us is perfect. I think all of us are going to have our own biases. We’re going to have our own personal values around how we think the world should be.”
From Dan Patrick’s message for seniors to lay down their lives to the chilling commentary from The Daily Telegraph, the world in mid-pandemic appears to be an uncomfortable place for people with more than six or seven decades of life behind them, particularly on the health front.
The question now is whether the ageism that has been exposed by a killer virus will prove to be the ultimate impetus for change in the way health systems and society treat its older members.
There are signs of hope. A small #caremongering Facebook group that sprung up in Toronto to help those in need has grown into a cross-country network of more than 9,000 members who deliver groceries and pick up prescriptions for housebound strangers, many of them seniors. Online, at least, compassion has gone viral.
A version of this article appeared in the July/August 2020 issue with the headline, “Has Ageism Become the New Eugenics,” p. 44.
RELATED:
Canada’s Hidden Shame: How COVID-19 Exposed Years of Systemic Neglect in Long-Term Care
Canadian Stars and Centenarians Shine During “Stronger Together, Tous Ensemble” Isolation Concert
How Some OECD Countries Helped Control COVID-19 in Long-Term Care Homes