The ER Diaries: Why Temporary Vision Loss Is Worth a Trip to the Doctor
A 78-year-old woman experienced a brief period of vision loss — and was diagnosed with having a mini-stroke or transient ischemic attack (TIA). Photo: RapidEye / Getty Images
Dr. Zachary Levine gives us the 911 on a 78-year-old woman who arrived at hospital after experiencing a brief period of vision loss — and was diagnosed with having a mini-stroke or transient ischemic attack (TIA). Here, how early medical intervention prevented a catastrophe.
The Case
A 78-year-old woman was gardening when suddenly she could not see out of her left eye. By the time the doctor saw her at a local clinic two hours later, her vision had returned to normal. He sent her to the ER for further assessment.
The Symptoms
The vision loss lasted 15 minutes and was painless. The patient enjoyed good health and did not smoke.
The Tests
The assessment of transient monocular vision loss begins with the details (painful or painless, complete or partial loss of vision, duration) and the person’s general health — older age is associated with some conditions like temporal arteritis, an inflammation of an artery that can cause vision loss, and blood supply problems are more likely in people with risk factors for atherosclerosis, such as smoking, high blood pressure, high cholesterol, or diabetes.
The patient was examined. Her vital signs (heart rate, oxygen saturation and temperature) were all normal, but her blood pressure was high — a cardiovascular disease (CVD) risk factor. Her eye examination revealed that the back of the eye (retina) appeared to be a bit pale, indicating suboptimal blood supply. The patient’s carotid arteries (large arteries on both sides of the neck that supply oxygenated blood to the brain) and the heart were also checked. A neurological examination followed, as a blood supply problem can affect the brain and cause other symptoms such as weakness, numbness, unsteady gait and difficulty speaking. All were normal.
An electrocardiogram (EKG) was done to test for an irregular heartbeat, which can increase the risk of blood clots. It showed a regular rhythm. Blood tests showed LDL (bad) cholesterol and elevated levels of glucose, showing that the patient had pre-diabetes, which put her at risk for developing full-blown diabetes. Next, a computerized tomography (CT) scan of the brain and neck arteries was performed, as was an echocardiogram (ultrasound of the heart). The CT scan showed a normal brain, but significant (more than 90 per cent) stenosis (narrowing) of the left carotid artery. The echocardiogram showed the heart was contracting well and regularly, with no blood clots present.
The Diagnosis
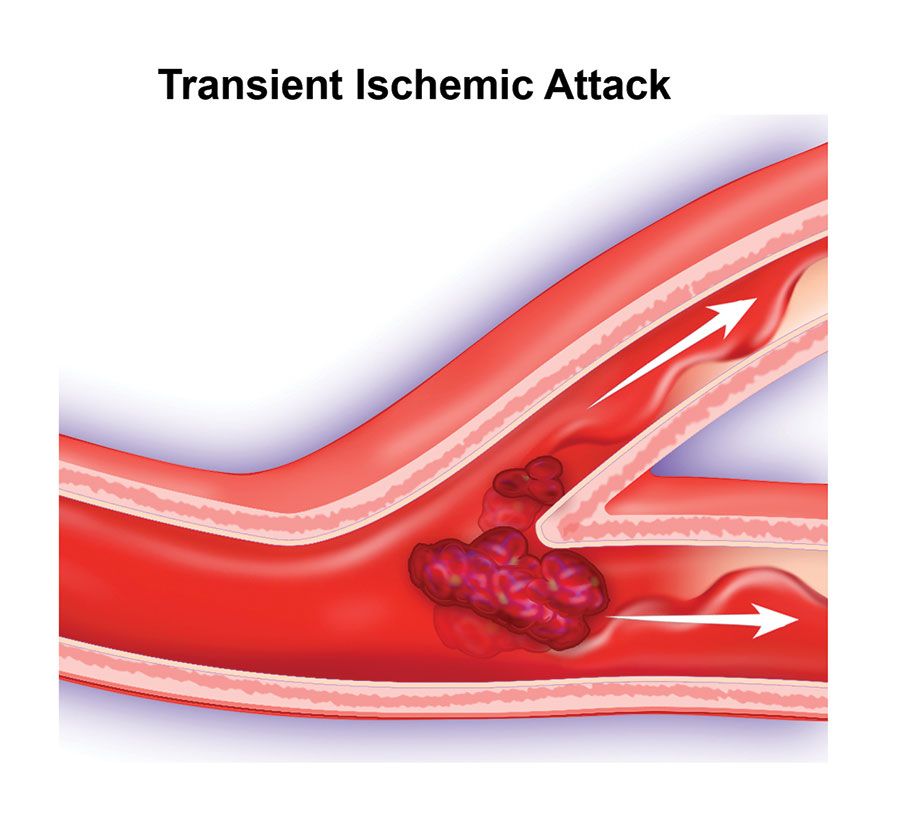
Transient vision loss — essentially a mini-stroke or transient ischemic attack (TIA), caused by lack of blood flow to the arteries supplying the eye — was confirmed. It usually results from atherosclerotic disease in the internal carotid artery, which can cause an embolus (an object such as blood clot or fatty deposit that moves in the bloodstream and blocks a small blood vessel) or stenosis (where the blood supply is compromised). Along with the evidence of CVD, it was a warning that the patient was at significant risk of a full-blown stroke, even though she had been feeling fine.
The Outcome
The patient received medical attention in time to prevent catastrophe. She underwent a carotid endarterectomy to clean out and open up the carotid artery. Her blood glucose, blood pressure and cholesterol are now managed with weight control, physical activity and medication, including a blood-thinning medication to further decrease her risk of ischemic stroke. She is back to gardening.
Dr. Zachary Levine is an emergency physician and associate professor in
the McGill University Department of Emergency Medicine.
A version this article appeared in the August/September 2021 issue with the headline “Zoomer Vitality: The ER Diaries: Dr. Zachary Levine Gives Us The 911,” p. 36.
RELATED:
The ER Diaries: Why a Change In Personality Is Worth a Trip to the Doctor
The ER Diaries: Why the Examination After a Fall Goes Beyond the Resulting Injury